Need support for a sprained ankle? Dive into our latest article for top recommendations
By Michael Christensen
What is a sprained ankle?
Ankle sprains are the most common lower limb musculoskeletal injury in sports and recreational activities. Lateral ankle sprains occur the most frequently and are often a result of an inversion (foot rolls in) and plantarflexion (foot tilts down) mechanism of action, which is associated with rapid change of direction, or rolling the ankle on uneven ground. Ankle sprains can cause pain, swelling, and weakness that can limit the ability to weight bear. In significant cases there may be neurological symptoms such as altered or reduced sensation.
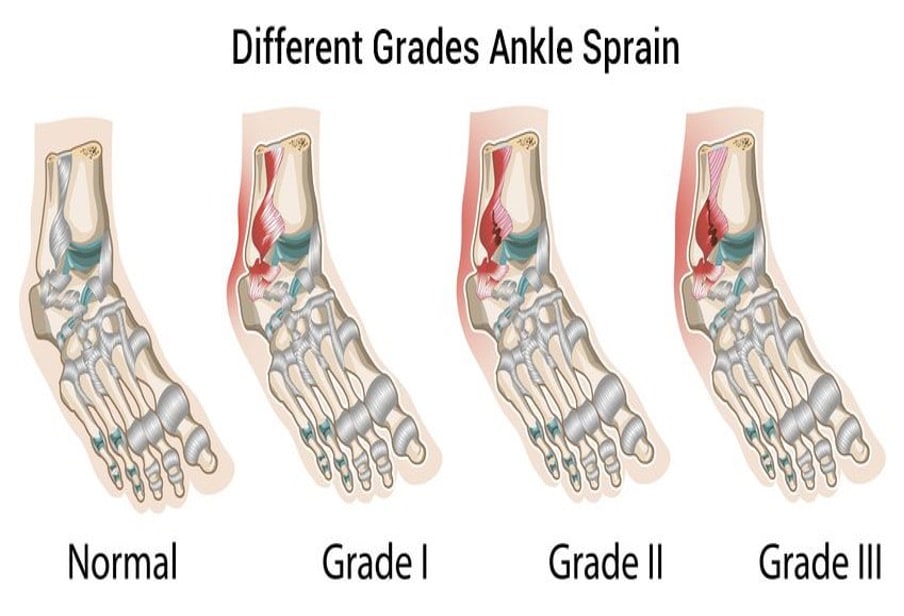
Ligament sprains are generally graded from 1 to 3, which relate to the amount of disruption of the ligament, with Grade 1 having minimal disruption, to Grade 3 being a complete disruption of the ligament. Ligaments play an important role in the stability of the ankle, and injury to them will result in a decrease in stability or “increased laxity” of the ankle joint.
The ATFL ligament and CFL ligament are the most involved in lateral sprains although severe cases can involve the ligaments higher up that form the syndesmosis or the ankle joint itself, which can result in a fracture of the distal fibula bone.
What to do if you roll your ankle?
Acute:
Management of an ankle sprain will depend on its severity. It is important to present to a first contact practitioner for an assessment, which could be the emergency department, your GP or a Physiotherapist.
The first consideration is to exclude a fracture, which can be done with the application of the Ottawa ankle rules, which are 99% sensitive at excluding a fracture if the result is negative. The Ottawa ankle rules take into consideration your ability to weight bear and tenderness on palpation of specific areas of the foot and ankle. If the rules are positive there is a clinical justification to refer for an Xray to help identify a fracture. Physiotherapists specialise in the assessment and management of the acute ankle sprain and can refer for imaging if indicated.
Once a fracture is excluded a physical assessment will help to identify the involved structures. There are several special tests that can help to test the stability of the ankle. Once the severity of the injury is identified, treatment plan can be conducted. In most cases there is indication for some support, which may range from taping or a soft cast, to a moon boot. Crutches may be prescribed to assist with mobilisation in the acute phase. Ice and elevation can be helpful to manage swelling. Early mobilisation is associate with reduced return to sport times.
Sub-Acute:
Once the ankle is less acute and able to tolerate more weight bearing it is important to further assess the strength and function of the ankle. Rehabilitation will typically involve a graded exercise program that will include strength, balance, and proprioceptive exercises.
Later stages:
Once sufficient strength and balance has been restored, rehab will transition towards tasks that are specific to the individual and their physical demands. Late-stage rehab will include things like balance, hopping, skipping, jumping, and running. The challenge of each exercise will gradually increase based on the tolerance of the ankle.
What happens if I manage it myself?
Physiotherapists are the most appropriate practitioners to assess and treat ankle sprains and are essential to guide rehabilitation and optimise your return to health and function. Ankle sprains often result in deficits to the strength and stability of the ankle, which can increase the risk of recurrent sprains if left unaddressed.
Graceville Physio have experienced clinicians who regularly treat ankle sprains. Give us a call on 3278 1186 to book an appointment or book online today.
Gaddi, D., Mosca, A., Piatti, M., Munegato, D., Catalano, M., Di Lorenzo, G., … & Bigoni, M. (2022). Acute ankle sprain management: an umbrella review of systematic reviews. Frontiers in Medicine, 9, 868474.