Respiratory Physiotherapy Brisbane
Frequently Asked Questions
What exactly does the respiratory physiotherapist do?
To begin with, your physiotherapist will assess the situation by listening to the chest and seeing how much movement occurs in the ribs and diaphragm. They can determine the airflow into the lungs and areas that are badly affected by mucus. Once they have a clearer understanding of your personal condition, they can begin to recommend exercises and treatment options that can help.
Some of these techniques are quite simple in theory. Some will recommend breathing exercises that can maximise the efficiency of your breath. This could have a big impact on oxygen intake. They can also advise on the best position to take to drain mucus from specific areas of the lung. This can ensure that drainage is more effective and doesn’t take as long.
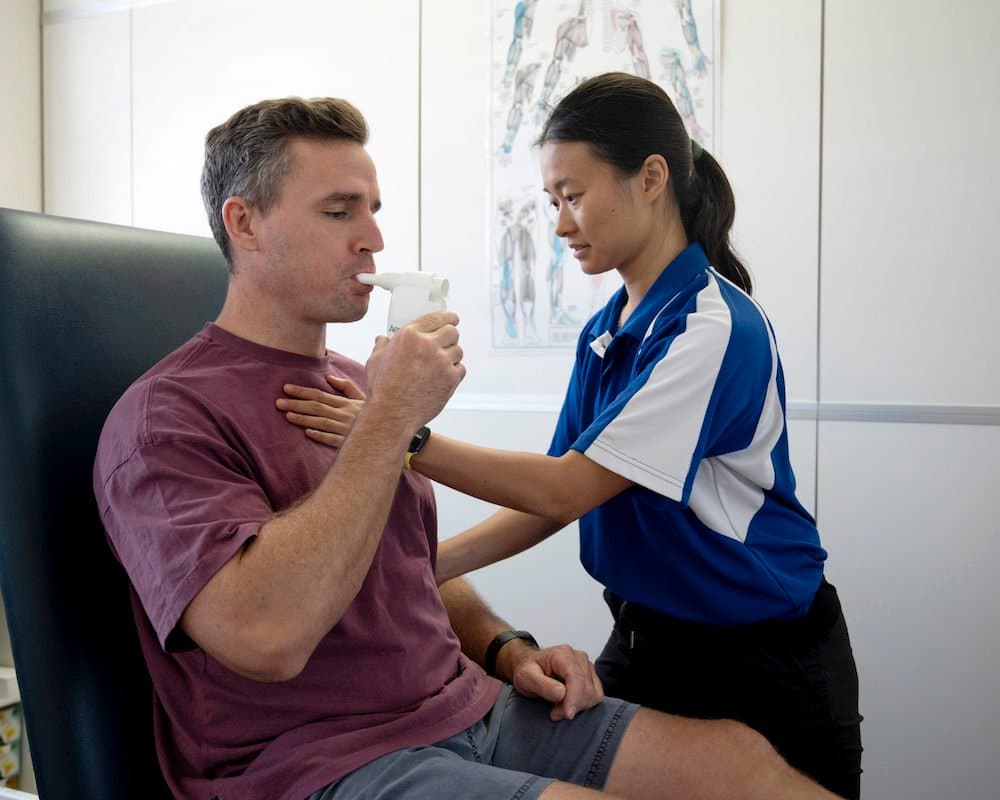
Many of these solutions are exercises that patients can complete at home. However, some people with severe impairments may benefit from the use of a specialist device. Positive Expiratory Pressure (PEP) therapy devices offer a different way to loosen and remove mucus from the lungs. Our chest physiotherapists can offer advice on these tools and help users get the best results.
What is chest percussion therapy?
Chest percussion is a common, hands-on physiotherapy treatment that can help patients with some of the illnesses mentioned above. Chest percussion requires several different measures to vibrate the chest and loosen the mucus.
Physios will use a drumming effect on the chest to shake the mucus free, but may also use other forms of vibration, deep breathing and coughing techniques to speed up the process. This can occur with the patient in a series of positions. The movement of the patient helps with drainage.
This is a skilled, intensive process, but one that can lead to great results.
How does physiotherapy help asthma?
This type of physio can help retrain your breathing, and strengthen your body. This helps the ease of breathing in general and reduces the likelihood of asthma attacks.
Why choose us for your Respiratory Physiotherapy
Graceville Physio is the ideal place to book a session with a respiratory physiotherapist. Our team are skilled in the techniques mentioned above and highly knowledgeable. This means an effective, professional service whether you require a few breathing exercises or intensive percussion of the chest.
They are also able to provide information on exercises for the home and any devices that may help. They are also friendly and personable, which is essential for these repeat, hands-on visits.
We have experts in respiratory physiotherapy that have gained experience by working in Respiratory wards that focus on these type of treatments. Contact us to find out more about chest physio in Graceville.






